A single-point rise in NEWS2 can signal trouble, yet many older patients deteriorate long before their numbers change. In England, about 35% of all people aged 65 and over live with some form of frailty, and roughly 69% of those aged over 85 live with multiple long-term conditions—both factors make early recognition tough. An infection might show up as new confusion rather than fever, and a fall might be the first sign of dehydration. These subtle shifts are easy to miss in busy UK care environments.
Deterioration is any decline in physical, cognitive, or functional status. It can appear suddenly, such as in acute respiratory compromise, or develop slowly over hours or days through reduced intake, increased sleep, or withdrawal.
This blog blends hard signs with soft signs to support sharper clinical judgement. The goal is simple: move from reacting late to acting early, using practical UK frameworks like SBAR to improve outcomes for older patients.
What is Meant by Deterioration?
When we talk about deterioration in an older patient, we mean a change from their usual physical, cognitive, or functional baseline. It is not always dramatic. In fact, it often starts quietly. You may see a patient who is a little more tired, a bit confused, or not walking as steadily as they did yesterday. These shifts may feel small, yet they often signal that something is beginning to go wrong.
Two Paths: Rapid vs Gradual Decline
Deterioration can unfold in different ways.
- Rapid or acute decline: This is the obvious type. You might see a sudden drop in oxygen levels, fast breathing, or a sharp change in consciousness.
- Gradual decline: This develops slowly, sometimes over days. A patient may eat less, sleep more, skip drinks, or move less. Although these signs seem mild at first, they often tell us the body is struggling.
Why Baseline Matters
Because older adults often present differently, knowing what is “normal” for the person becomes essential. For example, a mild temperature rise may be meaningful for someone who usually runs cold, and a small change in speech may signal the start of delirium. So, when you compare each sign to the patient’s baseline, you gain a clearer picture.
Why Recognising Deterioration Matters in Aged Care
Recognising deterioration early is one of the most important parts of caring for older adults. Although the first signs may appear small, they can signal the start of a serious decline. When we act early, we protect health, independence, and dignity. When we act late, the risks grow quickly.
The High Stakes in Older Adults
Older patients often have frailty, long-term conditions, or reduced reserves. Because of this, even a small change can lead to rapid decline.
Why this matters:
- The body compensates less effectively.
- Illness presents differently, so warning signs are subtle.
- Delays can turn a manageable issue into a medical emergency.
How Early Recognition Improves Outcomes
When we spot deterioration early, we give patients a better chance of staying well.
Early action can lead to:
- Fewer avoidable hospital admissions
- Lower risk of complications (delirium, dehydration, pressure damage)
- Better mobility and confidence
- More stable long-term health
- Less distress for families and caregivers
Even simple steps, such as encouraging fluids, increasing observations, or reviewing medication, can change the trajectory.
The Risks of Missing Early Signs
If deterioration goes unnoticed, the patient may become harder to stabilise. Although this can happen quickly, it is often preventable.
Late recognition often results in:
- Longer hospital stays
- Increased falls
- Higher infection risk
- Loss of independence and daily functioning
- Emotional strain for families
Supporting Quality of Life
Beyond clinical outcomes, quality of life is a central goal in aged care. When we catch problems early:
- Patients remain comfortable
- They stay more engaged and mobile
- We avoid unnecessary disruption and distress
Why is Early Detection Important?
Early detection gives us a valuable head start. Although deterioration can look subtle in older patients, those first small changes often carry the biggest message. When we notice them early, we can act before the situation becomes unsafe. This makes care smoother for patients and easier for staff.
Preventing Rapid Decline
Older adults can move from stable to unwell far quicker than expected. Because their reserves are lower, even mild illness can trigger a chain reaction.
Early detection helps you:
- Interrupt problems before they escalate
- Avoid sudden medical crises
- Reduce the need for urgent transfers or hospital admissions
Reducing Hospital Admissions and Complications
Admissions can be tough for older people. They may face confusion, pressure injuries, or loss of mobility during a hospital stay. However, early detection often stops these outcomes.
When you act early, you are more likely to:
- Treat issues in place
- Avoid delirium caused by unfamiliar environments
- Prevent dehydration or infection from worsening
- Maintain stability and routine
Supporting Better Decision Making
When we catch change early, we can plan care more clearly. This includes talking with families, reviewing medication, or updating care plans. Although these steps may seem simple, they guide safer decisions.
Early detection leads to:
- More accurate assessments
- Better clinical judgement
- Timely escalation using frameworks like SBAR
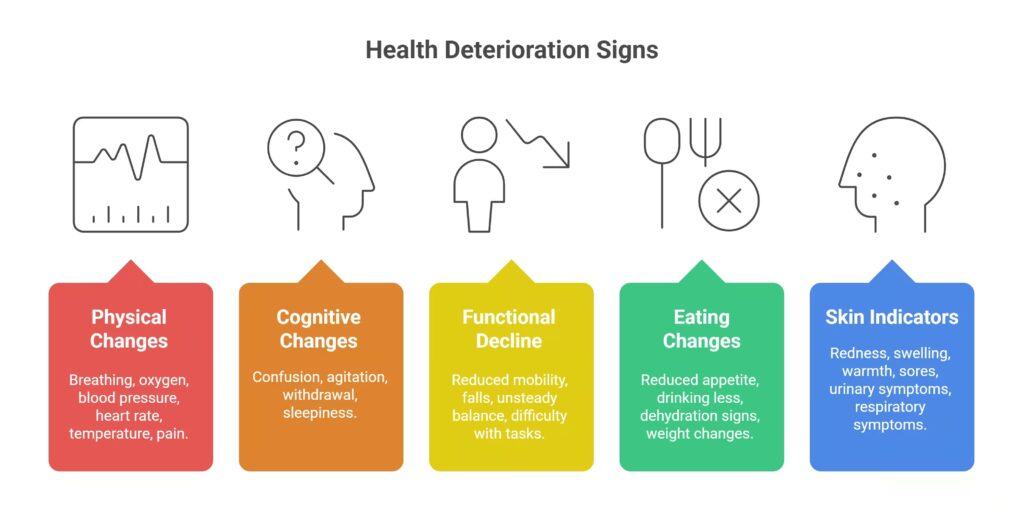
Common Signs of Health Deterioration in the Elderly
Recognising deterioration in older adults starts with noticing changes from their usual baseline. Although some signs are obvious, many are quiet and easy to overlook. When we stay alert to both physical and behavioural changes, we can act sooner and prevent avoidable decline.
Physical Changes You Should Not Ignore
Physical changes are often the clearest warning signs, yet in older adults they may be softer or slower to appear. Although you may not see dramatic shifts, even small changes can indicate that the body is under strain.
Look out for:
- Breathing changes: Faster breathing, shallow breaths, or new breathlessness often signal infection, heart failure, or reduced oxygen levels. Even a slight increase in respiratory rate is important, because it is one of the most reliable early indicators of deterioration.
- Oxygen level changes: A drop in oxygen saturation, even by a small margin, can be meaningful in frail patients. While it may not trigger a high NEWS2 score straight away, the trend matters.
- Blood pressure drops: New dizziness, light-headedness, or collapse can point to dehydration, infection, or internal bleeding. This is especially important in older people who already have postural blood pressure changes.
- Heart rate changes: A rising or irregular heart rate often shows early stress. It may appear before fever, pain, or oxygen changes become obvious.
- Temperature changes: Older adults may not mount a strong fever. Sometimes a very mild rise, or even a lower-than-normal temperature, is the first clue of infection or sepsis.
- New or worsening pain: Chest, abdominal, back, or unexplained pain should be taken seriously because older adults can mask symptoms or describe pain differently.
Although each of these signs may seem small, they often represent the first physical shift before a more visible decline.
Cognitive and Behavioural Changes
Cognitive changes are some of the earliest and most reliable indicators of deterioration in older adults. Although these changes may appear subtle, they often show before any change in vital signs.
Common early clues include:
- New confusion or disorientation: This is one of the strongest indicators of acute illness in older patients. Even mild confusion or slower responses may signal infection, dehydration, or medication issues.
- Sudden agitation or irritability: Behavioural shifts often reflect discomfort, pain, or fear. Although agitation can be dismissed as “just behaviour,” it usually points to something deeper.
- Withdrawal from normal activities: If a patient who normally chats, joins activities, or engages with others suddenly becomes quiet or detached, this can indicate early decline.
- Increased sleepiness: Sleeping more than usual, especially during the day, may signal infection, low oxygen, or metabolic issues. Even though tiredness seems minor, it often appears before physical signs.
Because these signs show through interaction rather than equipment, you may notice them during everyday moments such as dressing, mealtimes, or medication rounds. You can read more in the NHS guidance on delirium.
Functional Decline
Older adults often show deterioration through a drop in functional ability. Although this is easy to overlook, it is one of the strongest early indicators that something is changing.
Watch for:
- Reduced mobility: Slower walking, heavier steps, or needing more support than usual often reveal pain, infection, or muscle weakness.
- Increased falls or near-falls: A single fall can be the first obvious sign of dehydration, infection, low blood pressure, or worsening frailty.
- Unsteady balance: Even a small change in steadiness can signal neurological issues, medication side effects, or cardiovascular strain.
- Difficulty with daily tasks: Struggling to wash, dress, or move from a chair may indicate cognitive decline, fatigue, or illness. Although these tasks are routine, a sudden change can be clinically significant.
These functional changes show how well the patient’s body is coping day to day, which makes them essential to recognise early.
Eating, Drinking, and Hydration Changes
Changes in eating and drinking are often early indicators that something is wrong. Although these signs seem simple, they carry a lot of clinical value.
Key signs include:
- Reduced appetite: If a patient who normally eats well begins to pick at food or avoid meals, it may indicate infection, pain, depression, or nausea.
- Drinking less: Lower fluid intake is common in older adults, but when it drops suddenly, it increases the risk of dehydration, low blood pressure, and confusion.
- Signs of dehydration: These can include dry mouth, strong-smelling urine, darker urine, headache, fatigue, or new dizziness.
- Sudden weight changes: Unplanned weight loss often shows worsening chronic illness or nutritional decline, while sudden weight gain may reflect fluid retention.
Although these signs seem everyday, they often appear before more serious symptoms.
Skin and Infection Indicators
The skin offers clues about underlying health. Older skin is thinner, heals slowly, and reacts quickly to stress, which makes these signs especially important.
Signs to monitor include:
- New redness or swelling: These may suggest infection, pressure injuries, or poor circulation. Early changes can progress quickly if ignored.
- Warmth or heat: Localised warmth can indicate inflammation or infection, even without fever.
- Sores or pressure areas: Pressure damage forms faster in frail patients and often opens the door to infection.
- Urinary symptoms: Increased frequency, stronger odour, or discomfort may signal UTI, which is a common cause of delirium in older adults.
- Respiratory symptoms: New coughs, increased sputum, or changes in breathing often point to early respiratory infection.
Because infections can present atypically in older adults, these skin and surface-level signs are highly valuable.
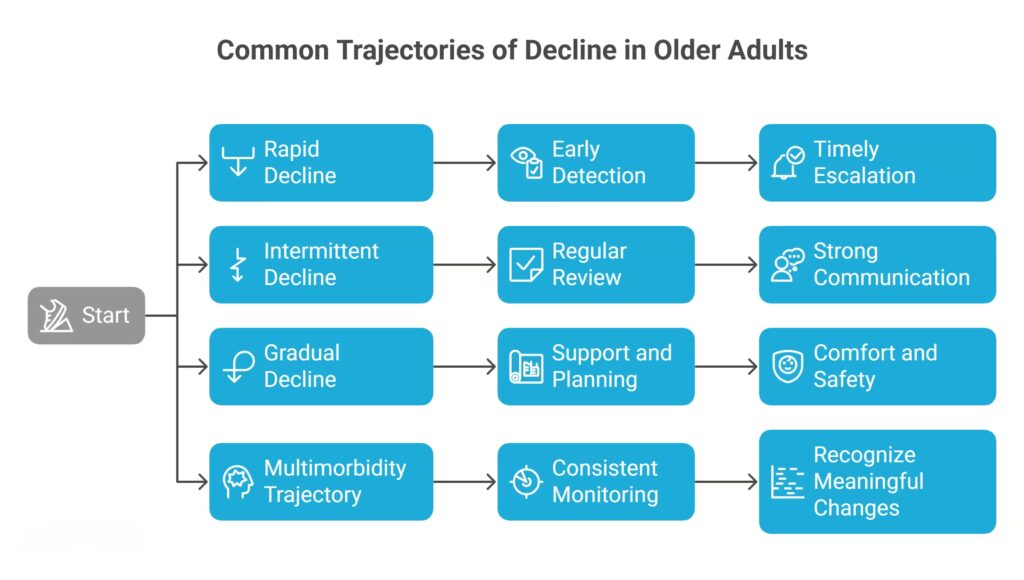
Common Trajectories of Decline
Older people do not all decline in the same way. Although the signs may look similar at first, the pattern or trajectory of decline often depends on the person’s main diagnosis, frailty level, and other long-term conditions. When you understand these trajectories, you can spot changes earlier and plan care more confidently. Below are the four most common patterns you will see in aged care.
Rapid Decline
Rapid decline happens suddenly. You may notice a sharp change in mobility, breathing, or cognition over hours or days. Although it can happen to anyone, it is more common in conditions like advanced cancer, severe infection, or acute stroke.
Key features include:
- A clear and fast drop in strength or alertness
- Sudden changes in vital signs
- A short period between being stable and being unwell
Because this trajectory moves quickly, early detection is essential. Even small concerns should prompt close monitoring and timely escalation.
Intermittent Decline
Some older adults follow a stop-start pattern. They appear stable for a while, then suddenly experience a dip, and then recover partially before the next episode. Although this can feel unpredictable, it often follows illnesses such as heart failure, COPD, or repeated infections.
What to watch for:
- Periods of stability followed by short bursts of deterioration
- Frequent hospital admissions or repeated episodes of the same problem
- Slower recovery after each dip
As these episodes continue, you will usually see the person return to a lower baseline each time. Because of this, regular review and strong communication between teams become especially important.
Gradual Decline
Gradual decline is slow and steady. Although the changes are small, they add up over months or years. You may notice reduced appetite, slower movement, or more fatigue long before anything appears in the observations.
Common signs include:
- Ongoing weight loss
- Reduced mobility or more frequent falls
- Cognitive changes that become clearer over time
- More dependence with daily tasks
Although this trajectory is subtle, noticing changes early helps you support comfort, safety, and planning.
Multimorbidity Trajectory
Many older adults live with more than one long-term condition, such as diabetes, dementia, arthritis, and heart disease. This mix creates a complex and unpredictable pattern. Decline may be triggered by minor issues like dehydration, medication changes, or infection.
What makes this trajectory different:
- Multiple conditions interacting with each other
- Atypical or confusing presentations
- Higher risk of rapid decline even from small stressors
- Difficulty returning to previous baseline
Because of this complexity, you often need to rely on soft signs as much as hard signs. Although the trajectory can seem unclear, consistent monitoring helps you recognise meaningful changes early.
Tools for Recognising Deterioration
When we care for older adults, tools help us pick up changes early and stay consistent in our assessments. Although experience and intuition still matter, structured tools give us clearer language, better documentation, and safer decision making. Below are the key tools you can use across aged care, community, and NHS settings.
1. SPICT
SPICT (Supportive and Palliative Care Indicators Tool) helps you identify people who are showing signs of worsening health or frailty. It is especially useful when someone is declining slowly and you want to understand the bigger picture.
SPICT helps you notice:
- Ongoing weight loss or reduced appetite
- Increasing frailty or more frequent falls
- Repeated infections
- Multiple hospital or GP visits
- Worsening long-term conditions
- Reduced ability to manage daily tasks
Although SPICT does not give a diagnosis, it helps you recognise patterns and prompts you to consider anticipatory care planning, supportive interventions, or closer monitoring.
2. NEWS2
The National Early Warning Score 2 is widely used in NHS hospitals, care homes, and some community services. Although older adults may sometimes present differently, NEWS2 still gives valuable objective data.
What NEWS2 tracks:
- Respiratory rate
- Oxygen saturation
- Blood pressure
- Pulse
- Temperature
- Level of consciousness
Because deterioration in older adults can develop before the score rises, you should use NEWS2 alongside soft signs and baseline knowledge. Even a one-point rise can be meaningful in frail patients.
3. Soft Signs Tools
Soft signs tools help you pick up the subtle early changes that often appear before vital signs shift. These are widely used in UK care homes.
Common soft signs include:
- More tired than usual
- Eating or drinking less
- New confusion or withdrawal
- Unsteady walking
- Not their “usual self”
Although these changes are often small, they are some of the strongest early indicators of deterioration. Soft signs tools help staff speak up confidently and escalate concerns sooner.
4. SBAR for Communication
Recognising deterioration is only half the job. You also need a clear way to report it.
SBAR (Situation, Background, Assessment, Recommendation) helps structure your communication so nothing important is missed.
SBAR supports you to:
- Explain what you see
- Give relevant history
- Share your assessment
- State clearly what you need
Although it is simple, SBAR often leads to faster and safer escalation.
5. RESTORE2 (for Care Homes)
RESTORE2 is a UK care-home tool designed to help staff spot deterioration early and communicate concerns effectively. It combines soft signs, NEWS2, and SBAR.
RESTORE2 includes:
- Early recognition prompts
- Soft signs checklist
- NEWS2 scoring
- SBAR communication guide
It is especially useful in care homes where clinical support may be limited.
6. Frailty Scales
Frailty tools help you understand a person’s baseline, which is critical when assessing deterioration.
Common tools include:
- Clinical Frailty Scale (CFS)
- Rockwood Frailty Index
When you know someone’s frailty level, you can identify meaningful deviations from their normal functioning more easily.
7. MUST (Malnutrition Universal Screening Tool)
Although not strictly a deterioration tool, MUST helps you spot nutritional decline, which is often one of the earliest signs that health is slipping.
MUST helps with:
- Weight tracking
- Appetite concerns
- Early nutritional interventions
Because nutrition affects everything from mobility to cognition, MUST supports early action.
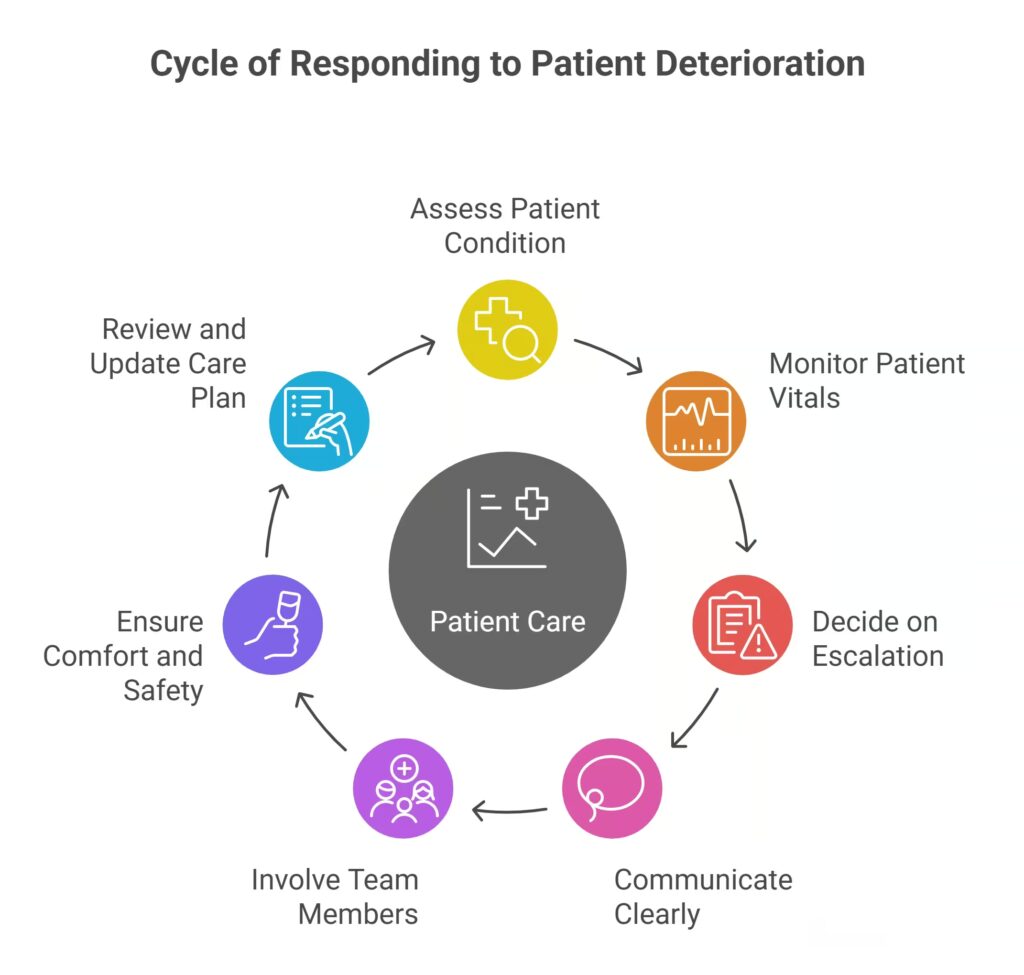
Responding to Signs of Deterioration
Recognising deterioration is only the first step. What you do next matters just as much. Although each situation is different, having a structured response helps you stay calm, act quickly, and keep the patient safe. When you combine your observations with clear communication and timely escalation, you reduce risk and improve outcomes.
1. Start With a Calm, Focused Assessment
Once you notice a change, take a moment to look at the whole picture. Even though the sign may seem small, it is safer to assume it matters.
Begin with:
- Rechecking observations such as pulse, breathing, and temperature
- Comparing the change to the patient’s usual baseline
- Looking for soft signs like confusion, reduced intake, or new weakness
- Asking the patient or family if anything feels “different”
Although these steps are simple, they help you avoid missing early clues.
2. Increase Monitoring and Write Everything Down
After your initial checks, you may need to observe the patient more often. This is especially important if the decline is new or unclear.
You can:
- Repeat vital signs at set intervals
- Track trends in eating, drinking, or mobility
- Note changes in behaviour or confusion
- Document all findings clearly and promptly
Good documentation helps the next person understand exactly what you saw and when you saw it.
3. Decide Whether Escalation Is Needed
Not all deterioration needs urgent medical intervention, but many cases do. Although the decision can feel complex, you can use tools and clinical judgement to guide you.
Consider escalation when you see:
- Worsening vital signs
- Sudden confusion or drowsiness
- Breathing changes
- Reduced urine output
- A fall with new symptoms
- Any “gut feeling” that something is not right
Even if you are unsure, it is safer to escalate early than to wait.
4. Communicate Clearly Using SBAR
Once you decide to escalate, how you communicate matters. SBAR helps you structure the information so the receiving clinician can understand the situation quickly.
SBAR supports you to share:
- Situation: What is happening right now
- Background: Relevant history or baseline
- Assessment: What you have found
- Recommendation: What you think is needed
Although SBAR is simple, it reduces miscommunication and speeds up response time.
5. Involve the Right Team Members
Because older adults often have complex needs, responding to deterioration is a team effort. You may need support from nursing staff, GPs, community teams, pharmacists, or emergency services.
The team can help with:
- Reviewing medication
- Providing guidance on monitoring
- Assessing risks like dehydration or infection
- Deciding whether hospital transfer is needed
Although you may start the process, you never respond alone.
6. Think About Immediate Comfort and Safety
While waiting for medical input, focus on keeping the patient safe and comfortable.
You might:
- Encourage fluids if safe
- Support positioning to help breathing
- Reduce noise or stimulation if confused
- Stay close and provide reassurance
Although small, these actions can prevent distress and improve stability.
7. Review and Update the Care Plan
Once the situation is under control, take time to review what happened. This helps you plan ahead and reduce future risks.
This review may involve:
- Updating baselines
- Adjusting care needs
- Reviewing nutrition or hydration plans
- Planning for closer monitoring
- Discussing next steps with family
Because deterioration often comes in patterns, this step is key to long-term safety.
If you want to build more confidence in spotting and reporting early changes, the Observation Skills for Carers course from HFOnline is a helpful next step. It covers practical observation techniques, soft signs, and escalation skills that support safer day-to-day care.
How to Support an Elderly Person Showing Signs of Deterioration
When an older person begins to deteriorate, they need calm, steady support. You do not need anything complicated. You just need a clear plan that keeps them safe, comfortable, and monitored while you arrange the next steps.
Stay Calm and Reassure Them
Your presence makes a real difference. When you speak slowly, keep the environment quiet, and reassure them that you are there to help, they usually feel safer and less anxious. This calm approach also helps you assess them more clearly.
Check Their Basic Needs
As deterioration begins, basic needs often slip. Simple actions like offering sips of water if it is safe, encouraging a light snack, helping them to the toilet, or adjusting their position can prevent further decline. These steps may feel small, but they help maintain stability while you observe them more closely.
Keep Them Safe From Falls or Weakness
Deterioration often brings unsteadiness, so safety becomes the priority. Staying nearby, keeping the area clear, and supporting slow, steady movements can prevent falls or sudden collapses. Even small moments of dizziness or confusion can lead to injury, so gentle supervision matters.
Keep Light Engagement Going
Talking to the person helps you understand how they are thinking and feeling. A short chat or a simple question can reveal early shifts in cognition or mood. When you help them with familiar items, such as glasses or hearing aids, you also reduce confusion and support clearer communication.
Involve Family or Regular Carers
Family members and regular carers often know the person’s baseline better than anyone. Asking whether the change is new or different gives you helpful context. Because deterioration is easier to spot when you know what “normal” looks like, their input can guide your next steps.
Prepare to Escalate
If the change continues or becomes more noticeable, it is important to act early. Informing senior staff, contacting the GP or community nurse, or using SBAR to pass on concerns ensures that the situation is taken seriously. Increasing observations can also help you track whether things are improving or getting worse.
The Simple Plan
Stay calm. Keep them comfortable. Keep them safe. Stay observant. Communicate early. Following this simple plan helps you support the person effectively while ensuring they receive timely and appropriate care.
Conclusion
Recognising deterioration in older adults is about noticing small changes and acting before they grow into bigger problems. When you stay alert to both hard signs and soft signs, you give every patient a safer and more stable path through illness.
With clear communication, early escalation, and steady, person-centred support, you move care from reactive to proactive. This approach protects health, preserves independence, and strengthens the quality of care across every setting.
Observation Skills for Carers
Frequently Asked Questions
You look for changes from the person’s usual baseline. This may include altered breathing, new confusion, reduced appetite, slower walking, or unusual behaviour. Even small shifts matter, because older adults often show subtle signs before vital signs change.
You know they are deteriorating when physical, cognitive, or functional changes appear together or progress over hours or days. Common examples include increased sleepiness, new unsteadiness, or sudden confusion.
Five common signs are:
- Breathing changes
- New confusion
- Reduced mobility
- Poor intake
- Behaviour changes
These usually show before the situation becomes urgent.
The 5 C’s are Compassion, Communication, Competence, Courage, and Commitment. They guide safe, respectful, and person-centred care.
The 8 standards usually include person-centred care, dignity, communication, safety, clinical effectiveness, timely care, coordination, and continuous improvement. They help ensure consistent, high-quality care.
Sudden decline is often caused by infection, dehydration, medication issues, acute illness, or a fall. Frailty makes older adults less able to cope, so changes can happen quickly.
They deteriorate quickly because they have lower reserves and often live with multiple conditions. This makes minor problems escalate faster than expected.
Soft signs include eating less, sleeping more, new confusion, withdrawal, or slower movement. These small clues often appear before vital signs change.
Stay calm, observe closely, compare changes to baseline, and escalate early using SBAR. While waiting for review, keep the person safe, comfortable, and monitored.
Useful tools include NEWS2, soft signs tools, RESTORE2, SPICT, and frailty scales. Using them together gives a clearer picture of early decline.
Table of Contents