The healthcare and social care sectors are experiencing an increasing demand for skilled professionals. According to recent studies, the global healthcare workforce shortage is expected to reach 10 million by 2030. With such challenges, online education is providing an accessible and flexible way for individuals to gain the necessary skills to make a difference.
Observation techniques are essential tools that every carer should master to improve patient outcomes. These techniques help carers identify changes in a person’s physical, emotional, or mental state, allowing for timely intervention and better care management. A skilled carer can make a significant difference through effective observation.
In this blog, you’ll learn about the key observation techniques every carer should know. We’ll cover practical methods for identifying early signs of distress or change, when and how often to observe, and how to record and act on your findings for better care outcomes.
What is Observation in Health and Social Care?
Observation in health and social care goes beyond just looking at someone—it’s about noticing changes in their physical, emotional, or mental state. By using all of our senses—sight, hearing, touch, and smell—we can identify signs of discomfort or health issues early on.
But why is observation so important? Well, our ability to notice even small changes can make a huge difference. For instance, a slight shift in someone’s mood or a subtle physical sign might be the first indication of a larger health concern. With effective observation, we can:
- Detect early signs of physical or mental health issues
- Recognize discomfort or pain, even when it’s not directly communicated
- Spot behavioural changes that may signal stress, anxiety, or confusion
Effective observation allows carers to take action quickly, ensuring the person in care receives the attention they need.
The Importance of Observation in Caring Roles

Observation is a key skill for anyone in a caring role. It helps us notice changes in a person’s health, emotions, or behaviour. By observing closely, we can act early to prevent problems and ensure the person gets the care they need. Here’s why it’s so important:
Prevents Health Problems
By observing small changes, like a slight increase in temperature or changes in movement, we can detect problems early. This helps us take action before things get worse, preventing health issues from escalating.
Improves Care Plans
When we observe how a person responds to their care, we can adjust their treatment if needed. This ensures that their care plan is tailored to their specific needs, helping them feel better and improving outcomes.
Helps with Communication
Some people may have trouble speaking about their feelings. Through observation, we can pick up on body language, facial expressions, or other signs that show how they are feeling. This helps us communicate and respond to their needs even when they can’t express them directly.
Keeps the Person Safe
Regular observation helps identify potential risks or hazards in a person’s environment. Whether it’s a trip hazard or noticing when someone is feeling unsteady, we can take action to make sure they are safe and avoid accidents.
If you want structured guidance on how to spot changes early and respond safely, the HF Online Observation Skills for Carers course gives step-by-step support. It’s especially useful if you’re new to care or want to refresh your existing skills.
What to Observe — Key Domains

As carers, it’s important to be aware of various aspects of the person’s condition. Observation isn’t just about looking at one area; we need to pay attention to different domains of health and behaviour. Below are key domains to observe when providing care.
1. Physical/Clinical Signs
Physical changes are often the first indicators of health problems. These can be visible or measurable signs that suggest something might be wrong.
- Vital signs: Monitoring things like heart rate, blood pressure, temperature, and breathing rate is crucial, especially for individuals with ongoing health conditions.
- Skin appearance: Check for rashes, bruises, or swelling, which can signal infections or injury.
- Mobility: Observe any changes in movement, such as difficulty walking, stiffness, or lack of coordination.
- Appetite and weight: Notice any changes in appetite or unintentional weight loss, which could indicate underlying issues.
- Pain: Look out for signs of discomfort, such as wincing, changes in posture, or reluctance to move certain body parts.
By keeping an eye on these physical signs, we can catch issues early and ensure timely medical intervention when necessary.
2. Behavioural & Emotional Cues
People express themselves in many ways, and as carers, we need to pay close attention to their behaviour and emotional state. These signs often reveal more than what words alone can tell us.
- Mood shifts: Watch for sudden changes in mood, such as feeling unusually sad, angry, or anxious, which could indicate emotional distress.
- Social withdrawal: If someone begins to avoid social interaction or seems unusually withdrawn, it might be a sign of mental or emotional health concerns.
- Agitation or confusion: Restlessness, irritability, or confusion could signal discomfort or cognitive issues, such as dementia or anxiety.
- Facial expressions and body language: Non-verbal cues, like a tense posture, frowning, or avoiding eye contact, can tell us a lot about how a person is feeling.
Observing these cues will help us understand what the person might be experiencing emotionally or mentally and allow us to offer the appropriate support.
3. Environmental & Social Context
The environment and social surroundings of the person can greatly affect their well-being. By observing their interactions with their space and others, we can identify if they are in a comfortable and safe environment.
- Safety hazards: Look for things like cluttered floors, poor lighting, or obstacles that might pose a risk of falling.
- Room conditions: Ensure that the person’s living area is clean, organized, and comfortable, as an uncomfortable or unhygienic environment can lead to stress or health problems.
- Social interaction: Pay attention to how they interact with others. Are they engaging in conversations? Are they showing signs of loneliness or distress when interacting with family members or carers?
- Routine: Observe if their daily routine is being maintained, or if there are changes in their habits (e.g., sleeping patterns or meal times) that might indicate a problem.
By observing both the environment and social context, we can identify changes that might impact a person’s well-being and address them promptly.
4. Patterns & Baseline vs Change
Understanding a person’s normal routine and behaviour is key to identifying when something is off. This is where baseline observations come into play.
- Establishing a baseline: Before we can notice changes, we need to understand what’s “normal” for the person. This could include their typical mood, eating habits, sleep patterns, and mobility.
- Tracking changes over time: Once you know their baseline, watch for patterns over time. For instance, if someone’s usual positive mood shifts to irritability over several days, this could signal an issue that requires attention.
- Recognising significant changes: Even small deviations from the baseline—such as a sudden loss of appetite or sleep disturbances—can be indicators of something more serious.
By continuously observing and comparing changes against their baseline, we can catch issues early, respond appropriately, and ensure the person’s health is being properly monitored.
Types of Observation in Health and Social Care
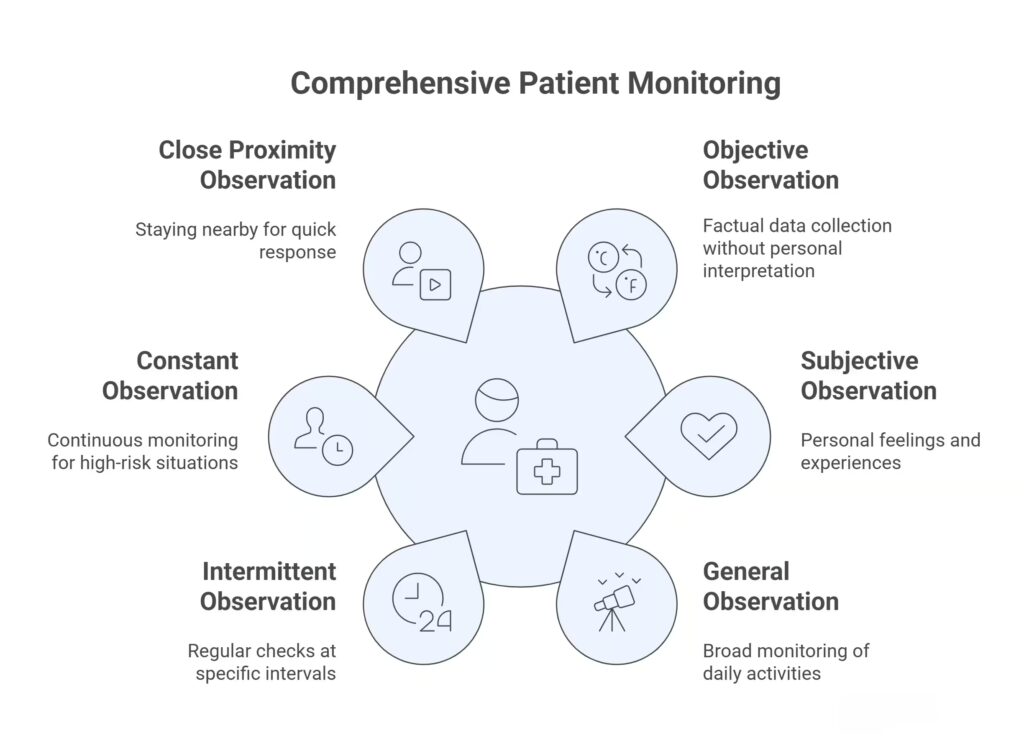
In health and social care, there are several types of observation that we use to monitor the well-being of those in our care. Each type of observation serves a different purpose and can be applied in various situations. Let’s look at the six key types of observation you should know about.
1. Objective Observation
Objective observation is all about facts. This type of observation focuses on what can be seen, heard, or measured without any personal opinions or interpretations. It is based purely on concrete data, which makes it a reliable way to document what’s happening.
- Examples: Recording a person’s temperature, heart rate, or blood pressure. Noting the color of a wound or the amount of food they ate.
- Why it’s important: Objective observations are factual and unbiased, ensuring that the information is accurate and can be used to make informed decisions.
2. Subjective Observation
Subjective observation, on the other hand, is based on personal feelings, perceptions, or experiences. This type of observation is more about what the person says or how they seem to feel. It’s important, especially when understanding emotional or mental health.
- Examples: Noting if a person seems anxious, sad, or in pain. Asking them how they feel and recording their response.
- Why it’s important: Subjective observations help us understand the person’s inner experience and emotional state, which can’t always be measured through objective data.
3. General Observation
General observation is a broad approach where we observe the person during their usual activities. This type of observation doesn’t focus on any specific issue but aims to give us an overall sense of how the person is doing.
- Examples: Watching how a person interacts with others, their daily routine, or their behaviour during routine activities like eating or walking.
- Why it’s important: General observations help us get a sense of the person’s general well-being and allow us to identify any areas that may need further attention.
4. Intermittent Observation
Intermittent observation involves checking on the person at specific intervals or times. It doesn’t require constant attention but ensures that the person is monitored regularly to catch any changes or issues.
- Examples: Checking on someone every 15 minutes, or once every hour, depending on their condition.
- Why it’s important: Intermittent observation allows carers to keep an eye on the person without needing to be constantly present. It’s useful for people who need regular but not continuous monitoring.
5. Constant Observation
Constant observation means watching a person without interruption. This type of observation is required when someone’s condition is unstable or when there’s a high risk of something going wrong.
- Examples: Monitoring someone who is at risk of falling, someone who is confused, or someone who might harm themselves.
- Why it’s important: Constant observation ensures the person is always being looked after and can receive immediate help if their condition worsens. It’s crucial for high-risk situations where timely intervention can make a significant difference.
6. Close Proximity Observation
Close proximity observation means staying near the person to watch them closely, often within arm’s reach. This type of observation is used when someone needs more than just a quick check-in but doesn’t require full-time monitoring.
- Examples: Staying within the same room or nearby when a person is unwell, confused, or at risk of falling.
- Why it’s important: Close proximity allows the carer to respond quickly if something changes, while still giving the person some space to maintain independence.
Each type of observation has its own purpose and can be used in different care situations. By understanding these six types, you can tailor your approach to fit the needs of the person you’re caring for, ensuring they receive the most appropriate level of monitoring and support.
Common Observation Techniques Carer Use
As carers, we use different techniques to observe and monitor the well-being of those we care for. These techniques help us gather valuable information and make sure we are responding to their needs in the best way possible. Let’s explore some of the most common observation techniques carers use.
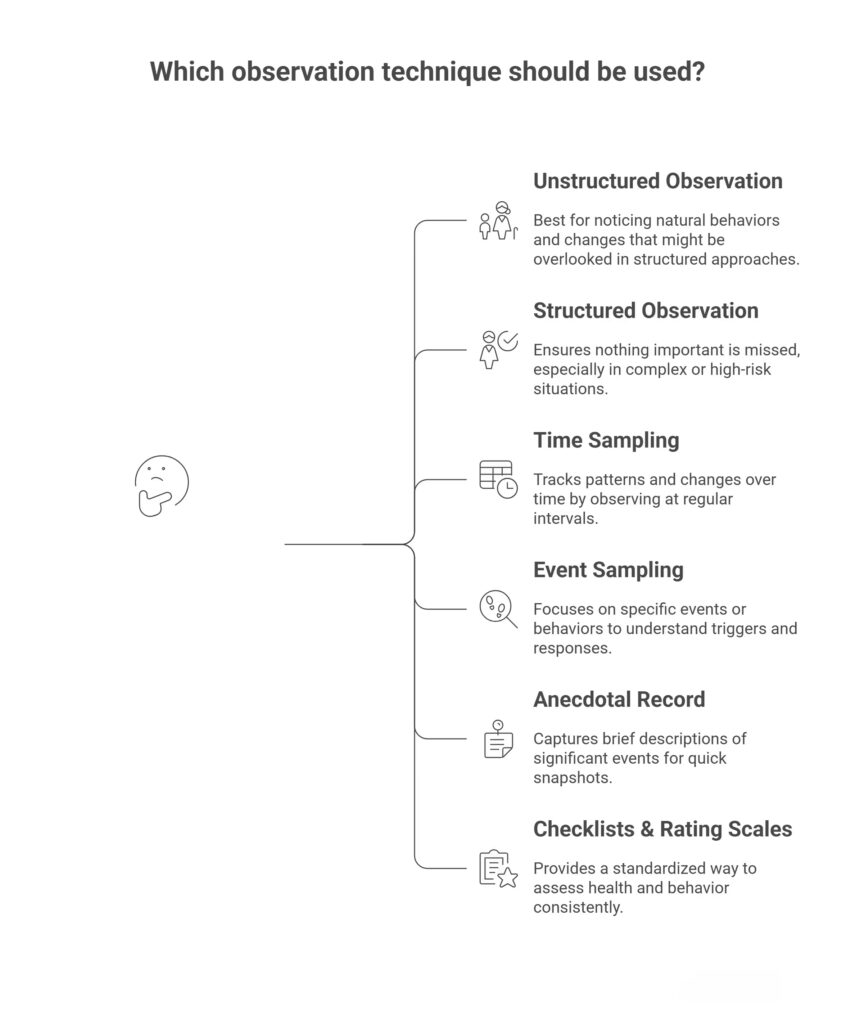
1. Unstructured Observation
Unstructured observation is the most natural form of observation. This technique involves simply watching a person during their normal activities without any set schedule or checklist. It’s about noticing any changes or signs that may arise as the person goes about their day.
- How it works: You observe the person during their daily activities—like eating, walking, or interacting with others—and pay attention to any changes or unusual behaviours.
- Why it’s important: It allows us to pick up on natural behaviours and changes that might otherwise be overlooked in a more structured approach.
2. Structured Observation
Structured observation is more planned and organised. In this technique, we observe a person based on a set of specific criteria or a checklist. This can include things like monitoring vital signs, checking mobility, or assessing mood.
- How it works: You follow a specific plan, observing the person at set times or checking for certain indicators, such as pain levels or ability to perform tasks.
- Why it’s important: Structured observation ensures that nothing important is missed, especially when dealing with a complex condition or high-risk situation. It also helps track progress over time.
3. Time Sampling
Time sampling involves observing a person at regular, predetermined intervals. This method is often used when carers need to keep track of changes over a period of time but don’t need to be constantly present.
- How it works: You check on the person at set times—such as every 10 or 15 minutes—and record observations based on what you see at that moment.
- Why it’s important: Time sampling helps track patterns and notice any changes over time. It’s great for monitoring progress or keeping track of someone’s behaviour or condition throughout the day.
4. Event Sampling
Event sampling focuses on specific events or behaviours. Instead of observing over time, this technique focuses on recording a particular event or behaviour when it occurs.
- How it works: You observe a specific event or behaviour, like a fall, agitation, or a change in a person’s mood. You then record everything about that event, including what led to it and how it was handled.
- Why it’s important: Event sampling helps carers understand the triggers and responses to specific behaviours. It’s especially useful when dealing with behaviours like aggression, confusion, or distress.
5. Anecdotal Record
An anecdotal record involves writing down brief, factual descriptions of significant events or behaviours. This technique helps carers keep track of important moments in a person’s day, focusing on key incidents.
- How it works: You write down short descriptions of noteworthy events, such as someone expressing discomfort or reacting to a change in routine.
- Why it’s important: Anecdotal records provide a quick snapshot of significant events, making it easier to track changes and discuss them with other team members. They are useful for capturing moments that don’t necessarily fit into a structured observation method.
6. Checklists & Rating Scales
Checklists and rating scales provide a standardised way of observing. These tools help carers assess various aspects of a person’s health and behaviour using a simple, organised format.
- How it works: You use a predefined checklist or rating scale to assess things like pain levels, mobility, mood, or other important aspects of care.
- Why it’s important: These tools help ensure that observations are consistent and thorough. They also make it easier to compare changes over time and share information with other care professionals.
To avoid these common mistakes, it can help to follow a structured training path. The HF Online Observation Skills for Carers course covers these pitfalls in detail and shows you how to handle them confidently.
Use of Technology & Monitoring Tools
Technology is transforming the way we care for others, making it easier to monitor health and respond to needs quickly. These tools help us track important health information and improve care by providing real-time updates. Let’s take a look at some of the key technology tools used in health and social care.
1. Wearable Health Devices
Wearable devices, such as smartwatches and fitness trackers, are designed to monitor key health indicators like heart rate, sleep, and activity levels.
- These devices alert carers when something unusual happens, such as a sudden change in heart rate or movement.
- They offer a continuous way to monitor health, which is especially helpful for people with chronic conditions.
2. Telehealth & Remote Monitoring
Telehealth tools allow for monitoring a person’s health remotely, reducing the need for frequent doctor visits.
- Devices like blood pressure cuffs or glucose meters send health data to carers or doctors, who can track the person’s condition from a distance.
- This method ensures that people receive regular monitoring without having to leave their homes, making healthcare more accessible.
3. Video Monitoring & Cameras
Video monitoring tools help carers keep a close eye on someone’s safety, especially if they require constant supervision.
- Cameras can be placed in key areas to monitor the person’s movements and send alerts if something unusual happens, such as a fall.
- This provides a way to ensure safety while also giving carers peace of mind, particularly for individuals with memory issues or who may wander.
4. Mobile Apps for Carers
Mobile apps designed for carers help track daily tasks, health updates, and reminders.
- These apps allow carers to manage medication schedules, track symptoms, and keep a record of appointments.
- They help carers stay organised and ensure they don’t miss important tasks or deadlines, improving overall care.
5. Electronic Health Records (EHRs)
Electronic Health Records (EHRs) store a person’s medical history and care information in one digital system.
- Carers and healthcare professionals can easily access and update the person’s health information, including treatment plans, medications, and test results.
- EHRs streamline communication between carers, doctors, and other healthcare providers, ensuring everyone has the most up-to-date information.
How to Record, Report and Act on Observations

Recording and reporting observations is just as important as making them. When we document clearly and share information at the right time, we help ensure the person receives safe and effective care. This process also keeps everyone on the same page, from carers to healthcare professionals. Let’s break down how to do it properly.
Record Your Observations Clearly
When you observe something, it’s important to write it down as soon as you can. This helps you avoid missing details or forgetting important changes.
What to include:
- Date and time of the observation
- What you saw, using simple and factual language
- Any changes from the person’s usual routine or baseline
- How the person responded, both physically and emotionally
- Any actions you took, such as offering comfort or notifying a colleague
Because accuracy matters, try to keep your notes objective. Instead of writing “the person looked upset,” write something like “the person was crying and avoiding eye contact.”
Report Changes Promptly
Once you record the observation, the next step is to report it. Even small changes can be important, so it’s better to share information early rather than wait.
Who to report to:
- A senior carer or supervisor
- A nurse or healthcare professional
- Family members, when appropriate and allowed
Use clear, simple language when reporting. Start with the main change you noticed, then briefly explain what you observed and what actions you took. This helps others understand the situation quickly.
Act on the Information
Observations only make a difference when we act on them. After you report, you may need to follow instructions, adjust care, or continue monitoring.
Common actions include:
- Increasing how often you check on the person
- Making changes to their routine, such as encouraging rest or fluids
- Supporting the person emotionally if they seem distressed
- Helping reduce risks, like removing hazards if the person seems unsteady
- Contacting medical support if symptoms worsen
Because care needs can change quickly, it’s important to stay alert and respond based on what you observe.
Common Pitfalls & How to Avoid Them
Even with the best intentions, carers can sometimes miss important details. By knowing the common pitfalls, we can stay alert and improve the quality of care we provide.
1. Making Assumptions
Assuming we know what’s happening can lead to mistakes.
Avoid it by: focusing on facts, asking questions, and checking the person’s usual baseline.
2. Overlooking Small Changes
Minor shifts in mood, mobility, or routine can signal bigger issues.
Avoid it by: recording small changes, watching for patterns, and sharing updates with your team.
3. Weak Documentation
Unclear notes make it harder for others to understand the situation.
Avoid it by: writing simple, timely, and factual notes with key details.
4. Delayed Action
Waiting too long to report changes can put the person at risk.
Avoid it by: reporting concerns quickly and following your care procedures.
5. Ignoring Emotional Cues
Focusing only on physical signs means missing emotional or social changes.
Avoid it by: paying attention to mood, communication, and social interaction.
Tips to Improve Observation Skills as a Carer
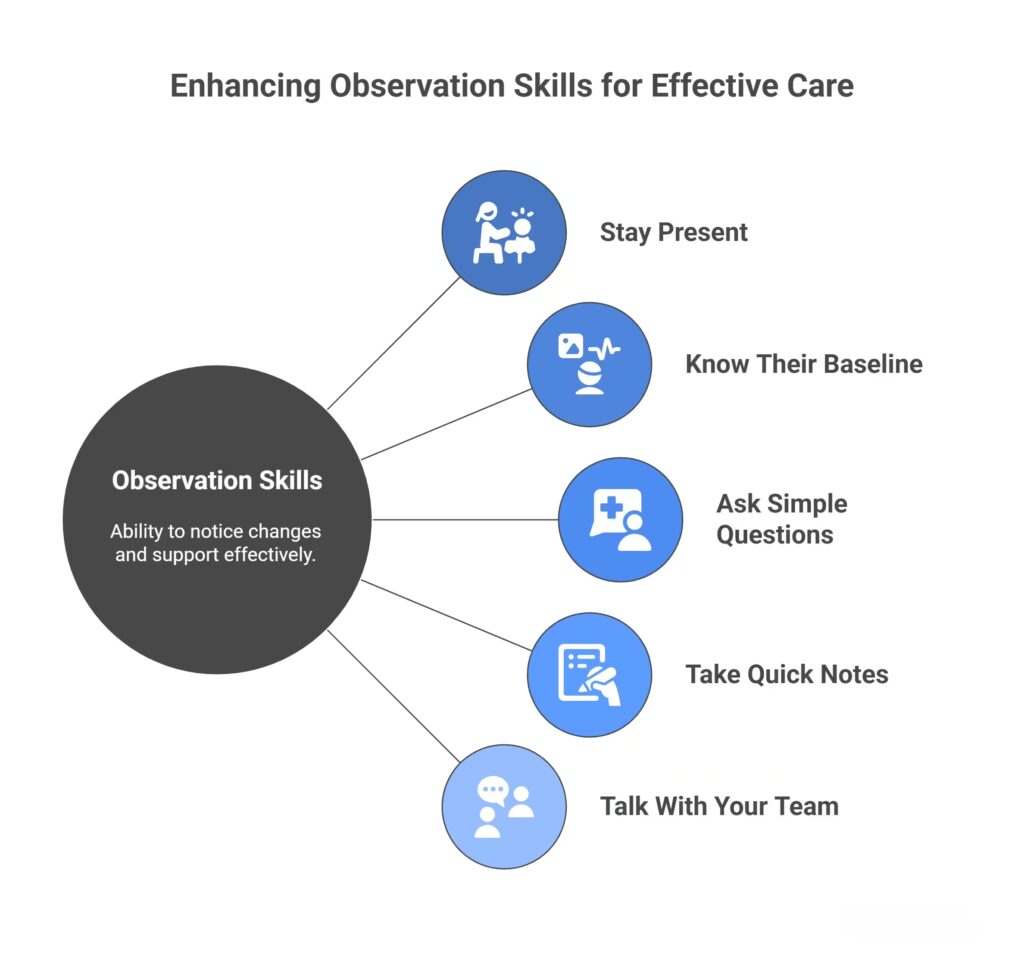
Strong observation skills help you spot changes early and support someone more effectively. Here are simple ways to build those skills.
Stay Present
When you stay focused, you notice more.
- Limit distractions.
- Observe before acting.
- Use all your senses.
Know Their Baseline
You understand changes better when you know what’s normal.
- Learn their routine and mood.
- Notice how they usually communicate.
Ask Simple Questions
People often share more when gently encouraged.
- Use easy, open-ended questions.
- Pay attention to tone and expressions.
Take Quick Notes
Notes help you remember details throughout the day.
- Write short reminders.
- Use checklists when needed.
Talk With Your Team
Sharing information strengthens care.
- Report early.
- Compare observations with others.
Small, consistent efforts like these can make your observation skills sharper and your care more effective.
Conclusion
Observation is one of the most powerful tools you have as a carer. When you stay alert and notice small changes, you help prevent problems and support the person more effectively. Every detail you pick up can guide better decisions and safer care.
As you continue to grow in your role, use the techniques and tips from this blog to strengthen your skills. With consistent practice, you’ll become more confident, responsive, and able to provide truly person-centred care.
If you’re ready to strengthen your skills and advance in your career, the Level 3 Diploma in Health and Social Care is a practical, flexible way to move forward. It’s built to support carers who want to make a bigger impact.
Observation Skills for Carers
Frequently Asked Questions
Observations in healthcare refer to the process of monitoring a person’s physical, emotional, and behavioural changes. Carers use their senses and various tools to notice signs of improvement or deterioration. These observations help guide decisions, prevent complications, and ensure the person receives timely and appropriate care.
The four commonly known observation techniques are objective observation, subjective observation, general observation, and structured observation. Each technique helps carers gather different types of information, ranging from factual details to behaviours or emotional cues.
In health assessments, observation techniques include watching physical movements, monitoring vital signs, noting emotional cues, checking skin appearance, and assessing communication patterns. Carers may also use tools like checklists, time sampling, and event sampling to make observations more accurate and organised.
The five basic clinical observations often monitored in care are:
Temperature
Pulse
Respiratory rate
Blood pressure
Oxygen saturation
These measurements help detect early health changes and guide necessary actions.
Observation is important because it helps carers notice both obvious and subtle changes in a person’s condition. By catching these changes early, we can prevent complications, adjust care plans, and support the person more effectively. It also helps maintain safety and improve communication between care teams.
Carers need strong attention to detail, patience, active listening skills, and the ability to stay calm under pressure. Knowing the person’s usual behaviour, routine, and baseline also helps carers identify changes quickly. Clear communication and good documentation are equally important.
How often you observe depends on the person’s needs. Some individuals only need general daily observation, while others may require intermittent or constant monitoring. Conditions such as dementia, recovery from surgery, or high fall risk may require more frequent checks.
Tools like checklists, digital apps, wearable devices, and electronic health records improve accuracy and organisation. These tools help track patterns, record information quickly, and share updates with the care team, making the observation process smoother and more reliable.
Carers should record the date, time, what they observed, any changes from the person’s baseline, and actions taken. Notes should be simple, factual, and free from personal opinions. This ensures other carers or healthcare professionals understand the situation clearly.
Carers can improve by staying focused, knowing the person’s baseline, taking notes, asking gentle questions, and communicating with the care team. Regular reflection on daily observations also helps identify areas for improvement and builds stronger overall awareness.