“Privacy is not something that I’m merely entitled to, it’s an absolute prerequisite.” – Marlon Brando. In any aspect of health and social care, patient data is very private and sensitive. Storing a large amount of medical records with a digital system, and protecting this information is not just a legal requirement—this is a moral obligation.
The General Data Protection Regulation (GDPR) enforces strict rules on handling patient data. It gives individuals control over their information while ensuring healthcare providers maintain transparency and security. Non-compliance can lead to severe penalties, making data protection a top priority in the sector.
In this blog, we will explain how GDPR safeguards patient data in health and social care. You’ll learn about its key principles, compliance measures, challenges, and how organisations can ensure data security while delivering quality care.
What is GDPR in Health and Social Care?
GDPR, or the General Data Protection Regulation, is a comprehensive data protection law that came into effect in the European Union (EU) on May 25, 2018. Although the UK has left the EU, GDPR principles have been incorporated into UK law through the Data Protection Act 2018. In health and social care, GDPR governs how patient data is collected, processed, stored, and shared. It ensures that healthcare providers handle sensitive information responsibly, with a strong emphasis on transparency, accountability, and patient rights.
Simply put, in the health and social care sector, GDPR requires organisations to have clear policies on data handling. Patients must be informed about how their data is used and have the right to access, correct, or delete it. This regulation also mandates strong security measures to prevent unauthorised access and misuse.
Understanding GDPR is essential for anyone working in health and social care. Gaining standard training—such as through the Health and Social Care Level 3 Diploma—can help professionals stay informed and compliant. In the next section, we’ll explore the key principles of GDPR and how they shape data protection in the industry.
Understanding GDPR and Its Core Principles
When you think about GDPR in health and social care, it really boils down to a set of clear rules. Rules designed to keep patient information safe and sound. These rules are based on seven core principles that ensure transparency, security, and accountability. Every organisation handling patient information must follow these principles to stay compliant and protect sensitive data.
GDPR is built on seven key principles that guide data protection practices:
- Lawfulness, Fairness, and Transparency – Data must be processed legally, fairly, and with full transparency. Patients should know how their data is used.
- Purpose Limitation – Information should only be collected for specified, legitimate purposes and not used beyond that scope.
- Data Minimisation – Organisations should only collect the necessary data needed for care, avoiding excessive or irrelevant details.
- Accuracy – Patient records must be kept up to date. Incorrect information can lead to serious consequences in healthcare.
- Storage Limitation – Data should not be stored longer than necessary. Healthcare providers must have retention policies in place.
- Integrity and Confidentiality (Security) – Strong security measures must be in place to prevent data breaches and unauthorised access.
- Accountability – Organisations must take responsibility for compliance, demonstrating how they follow GDPR requirements.
These principles shape how patient data is collected, stored, and shared in health and social care. They ensure that personal information stays secure and is used only for the reasons it was collected in the first place.
Key Principles of GDPR in the Context of Patient Data Protection
GDPR provides a strong legal framework to ensure that patient data is handled carefully. In health and social care, data security is important because it includes very sensitive information, including medical history, diagnosis and treatment plans. Using GDPR’s main principles specifically on patient data strengthens privacy and security, and ensures moral data management.
- Patient Consent and Control – Healthcare providers must obtain clear and informed consent before collecting or processing patient data. Patients also have the right to withdraw consent at any time.
- Data Confidentiality and Security – Medical records must be protected from unauthorised access. This requires encryption, secure storage, and restricted access to authorised personnel only.
- Transparency and Access Rights – Patients have the right to know how their data is used. They can request access, updates, or deletion of their records when necessary.
- Purpose Limitation in Medical Use – Data should only be used for providing healthcare services and improving patient care. It cannot be repurposed without valid justification.
- Minimisation of Collected Data – Only essential patient information should be collected and stored. Unnecessary details increase security risks.
- Accuracy and Timely Updates – Outdated or incorrect medical data can lead to misdiagnosis or improper treatment. Regular reviews and updates are necessary.
- Data Retention and Lawful Disposal – Healthcare providers must have clear retention policies, ensuring records are kept only for the necessary period before secure disposal.
- Accountability and Compliance – Organisations must demonstrate compliance through proper documentation, audits, and adherence to security protocols.
Types of Sensitive Data in Healthcare
Healthcare deals with some of the most sensitive categories of personal data, known as “special category data” under GDPR. This includes:
- Medical history and diagnoses
- Treatment plans and prescriptions
- Genetic and biometric data
- Mental health records
- Social care needs and support plans
Such data requires the highest level of protection due to its potential to cause harm if misused or exposed.
Health and Social Care Level 3 Diploma
What Are the GDPR Requirements for Healthcare Providers?
Healthcare providers handle some of the most sensitive personal data, making GDPR compliance a legal and ethical necessity. To achieve this, healthcare organisations must adhere to strict requirements regarding the collection, storage, and processing of patient data, all while maintaining complete transparency and accountability. Here are some of the actions that healthcare organisations must do for compliance.
1. Obtain Clear and Informed Consent
Before collecting patient data, healthcare providers must obtain explicit consent. Patients should understand how their data will be used, and they have the right to withdraw consent at any time.
2. Ensure Lawful Processing of Data
GDPR allows data processing without consent under specific conditions, such as when it is necessary for medical treatment, public health reasons, or legal obligations. However, providers must justify such processing and document their reasons.
3. Appoint a Data Protection Officer (DPO)
Healthcare organisations that process large amounts of sensitive data must appoint a Data Protection Officer (DPO). The DPO oversees GDPR compliance, advises staff, and acts as the main contact for data protection authorities.
4. Implement Strong Data Security Measures
Medical records must be protected using encryption, access controls, and secure storage. Only authorised personnel should have access to sensitive patient data, and cybersecurity measures must be in place to prevent breaches.
5. Maintain Transparency and Patient Rights
Patients have the right to access, correct, or delete their personal data. Healthcare providers must provide clear privacy notices explaining how data is collected, stored, and used.
6. Conduct Regular Data Protection Impact Assessments (DPIAs)
When introducing new data processing activities, organisations must conduct Data Protection Impact Assessments (DPIAs) to identify potential privacy risks and implement safeguards.
7. Ensure Secure Data Sharing and Transfers
Sharing patient data with other healthcare providers or third parties must follow strict security protocols. If data is transferred outside the EU, safeguards such as encryption or binding legal agreements must be in place.
8. Report Data Breaches Immediately
If a data breach occurs, healthcare providers must report it to the relevant authorities within 72 hours. If the breach poses a risk to patients, they must also be informed promptly.
9. Limit Data Retention and Disposal
Healthcare providers should only retain patient data for as long as necessary. When data is no longer needed, it must be securely deleted or anonymised to prevent misuse.
10. Demonstrate Accountability and Compliance
Organisations must document their GDPR compliance efforts, including policies, training records, and security measures. Regular audits help ensure that best practices are followed.
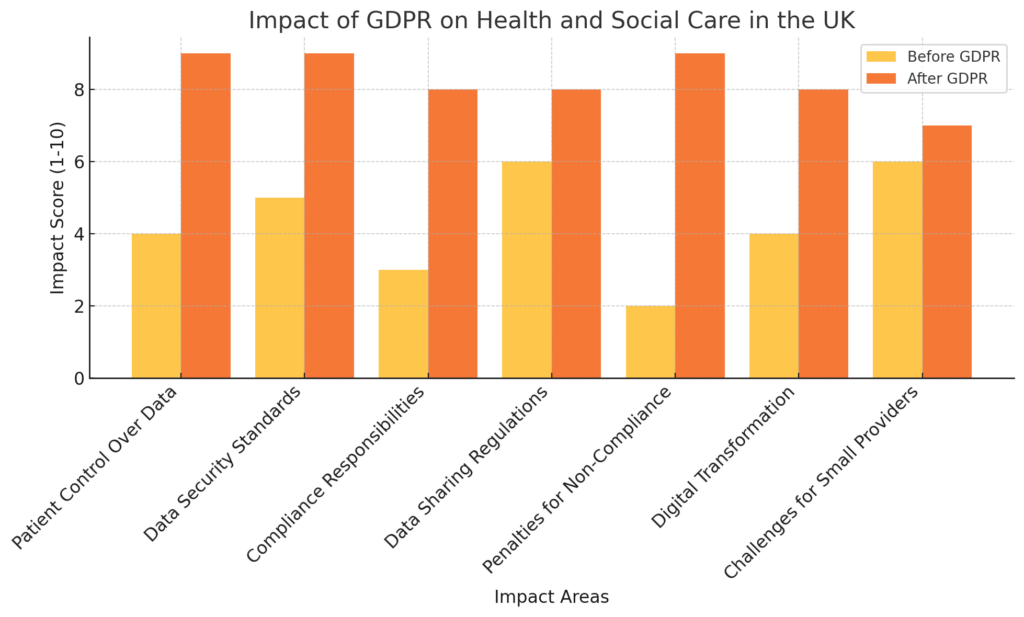
GDPR’s Impact on Health and Social Care in the UK
GDPR has transformed how patient data is handled in the UK’s health and social care sector. By enforcing stricter rules on data protection, it has improved privacy, security, and transparency. However, compliance has also introduced challenges, requiring healthcare organisations to rethink their data management practices.
1. Stronger Patient Rights and Control
One of the most significant impacts of GDPR is the empowerment of patients. Individuals now have greater control over their personal data, including the right to access, correct, and even request the deletion of their medical records. This has increased transparency and trust in healthcare providers.
2. Improved Data Security Standards
GDPR has pushed healthcare organisations to strengthen their security measures. Hospitals, GP practices, and care providers must now use encryption, access controls, and secure storage systems to protect sensitive patient data. Cybersecurity threats remain a concern, but GDPR has made organisations more proactive in preventing data breaches.
3. Increased Compliance Responsibilities
Healthcare providers must ensure they process patient data legally and fairly. The requirement to appoint a Data Protection Officer (DPO) for large-scale data processing has added an extra layer of accountability. Additionally, organisations must conduct Data Protection Impact Assessments (DPIAs) when implementing new systems or data-sharing practices.
4. Stricter Regulations on Data Sharing
Health and social care services often involve multiple agencies, including hospitals, care homes, and local authorities. GDPR has introduced stricter rules on data sharing, ensuring that personal information is only exchanged when necessary and with proper security measures in place. While this has improved patient confidentiality, it has also made cross-agency collaboration more complex.
5. Heavier Penalties for Non-Compliance
Under GDPR, healthcare organisations face severe penalties for data breaches or non-compliance. The Information Commissioner’s Office (ICO) can issue fines of up to £17.5 million or 4% of annual global turnover, whichever is higher. This has encouraged healthcare providers to prioritise compliance and invest in better data protection strategies.
6. Digital Transformation and Modernisation
To meet GDPR standards, many healthcare providers have had to upgrade their IT systems and adopt digital solutions that improve security and efficiency. This has led to the development of more secure electronic health records (EHRs), better patient portals, and improved data management processes.
7. Challenges for Smaller Healthcare Providers
While large hospitals and NHS trusts have the resources to meet GDPR requirements, smaller healthcare providers, such as private clinics and care homes, often struggle with compliance due to limited budgets and technical expertise. This has led to increased demand for GDPR training and consultancy services in the sector.
Best Practices for Data Protection in Healthcare
Protecting patient data is a legal and ethical responsibility for healthcare providers. Following best practices ensures compliance with GDPR while maintaining trust and security.
- Implement Strong Access Controls – Limit access to patient data to authorised personnel only. Use multi-factor authentication (MFA) and role-based permissions to prevent unauthorised access.
- Encrypt and Secure Data Storage – Encrypt sensitive patient data, whether stored digitally or shared electronically. Secure physical records in locked cabinets and restrict access.
- Conduct Regular Staff Training – Educate healthcare professionals on GDPR requirements and data protection best practices. Regular training reduces human errors that lead to breaches.
- Use Secure Communication Channels – Emails, patient portals, and digital health records should be encrypted to prevent data leaks. Avoid sharing sensitive information via unsecured channels.
- Perform Data Protection Impact Assessments (DPIAs) – Before adopting new technologies or processes, assess potential data security risks and take necessary precautions.
- Ensure Timely Data Disposal – Follow data retention policies and securely delete or anonymise patient records that are no longer needed.
- Monitor and Respond to Data Breaches – Have a breach response plan in place. If a data breach occurs, report it within 72 hours and take immediate corrective action.
By adopting these best practices, healthcare providers can strengthen patient data protection and ensure GDPR compliance.
What to Do If There Are Signs of a Data Breach in Your Healthcare Organisation
If a data breach is suspected, healthcare providers must act quickly to minimise damage and protect patient information. Here’s what to do:
1. Contain the Breach
Identify and isolate the affected system immediately to prevent further data leaks. This helps protect the rest of the network and limits the impact.
2. Assess the Impact
Determine what data was compromised and how it might affect patients. Understanding the extent of the breach helps in deciding the next steps.
3. Report to the ICO
If the breach poses a risk to individuals, it must be reported to the Information Commissioner’s Office (ICO) within 72 hours.
4. Inform Affected Individuals
If the breach could harm patients, notify them quickly. Provide clear details on what happened, what risks they face, and what actions they can take.
5. Investigate and Strengthen Security
Find out what caused the breach and fix the issue. Implement stronger security measures to prevent future incidents.
Quick action helps reduce damage and maintains trust in healthcare services.
Consequences of Non-Compliance with Data Protection Laws
Failure to comply with data protection regulations, specifically GDPR, can result in significant repercussions for healthcare organisations.
- Financial Penalties: Organisations may be subject to substantial fines, potentially reaching up to €20 million or 4% of their global annual turnover, whichever is greater.
- Reputational Damage: Moreover, data breaches and non-compliance can severely erode patient trust and damage an organisation’s reputation, leading to long-term consequences.
Legal Liability: Additionally, affected individuals may pursue legal action against organisations that fail to adequately protect their data, resulting in further financial and legal burdens.
Final Words
GDPR has reshaped how patient data is protected in health and social care, setting a clear standard for transparency and security. While compliance presents ongoing challenges, it’s also a foundation for building trust with patients and service users. Experts stress the importance of continuous staff training, strong security protocols, and well-defined data policies in upholding these standards.
As digital tools evolve, healthcare organisations must stay proactive—investing in secure systems and ethical data practices to meet new demands. For professionals looking to deepen their understanding and stay compliant, courses like the Health and Social Care Level 3 Diploma can provide valuable knowledge and support. Prioritising patient privacy isn’t just about meeting regulations—it’s central to delivering safe, reliable, and respectful care.
Frequently Asked Questions
The General Data Protection Regulation (GDPR) treats health data as a special category of personal data, meaning it gets extra protection. Whether it’s medical records, treatment details, or even appointment history, GDPR ensures this sensitive information is handled securely and lawfully.
Confidential information about service users or patients should be treated confidentially and respectfully. Members of a care team should share confidential information when it is needed for the safe and effective care of an individual.
Under GDPR, Data Protection Officers (DPOs) are responsible for ensuring organisational compliance with data protection laws. Their role involves monitoring data handling practices, supporting data protection impact assessments, raising awareness among employees, providing staff training, and maintaining communication with regulatory authorities when required.
The GDPR applies strict rules for processing data based on consent. The purpose of these rules is to ensure that the individual understands what he or she is consenting to. This means that consent should be freely given, specific, informed and unambiguous by way of a request presented in clear and plain language.
The GDPR is built on seven fundamental principles: lawfulness, fairness, and transparency; purpose limitation; data minimisation; accuracy; storage limitation; integrity and confidentiality; and accountability. These principles shape how organisations collect, manage, and protect personal data across all sectors.
Data protection is everyone’s responsibility. While a Data Protection Officer may lead compliance efforts, all staff members who handle personal data have a duty to process it securely, ethically, and in line with the organisation’s Data Protection Policy.



















